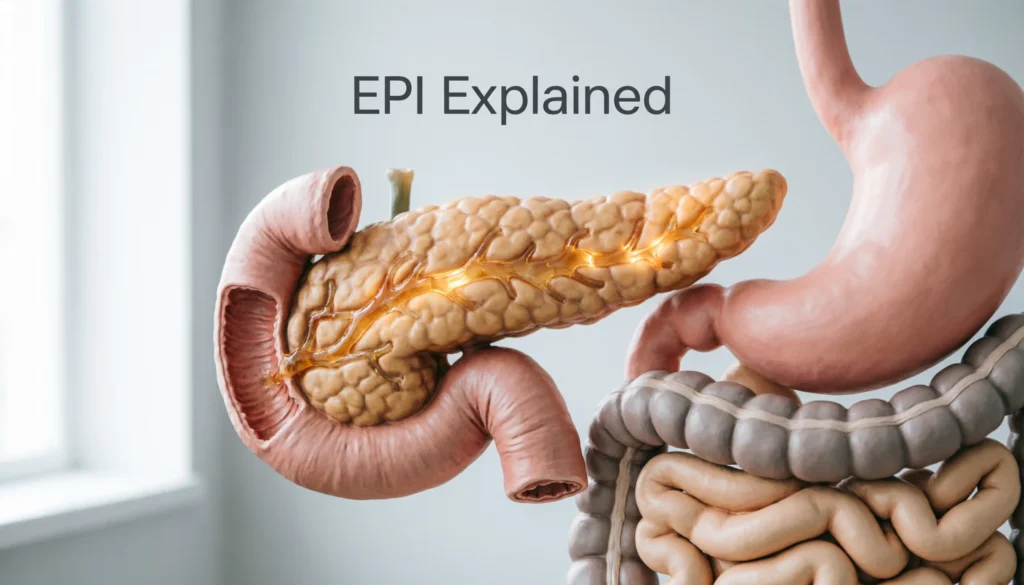
EPI in medical terms stands for Exocrine Pancreatic Insufficiency, a condition in which the pancreas does not produce enough digestive enzymes to properly break down food, leading to malabsorption, nutrient deficiencies, and digestive discomfort.
Understanding EPI is essential for anyone experiencing chronic digestive issues, unexplained weight loss, or nutrient deficiencies. With timely diagnosis and treatment, many of the symptoms of EPI can be effectively managed, improving overall health and quality of life.
Origin and Meaning of EPI
The abbreviation EPI is derived from the following medical terms:
- Exocrine – relating to glands that secrete substances through ducts, rather than into the bloodstream
- Pancreatic – relating to the pancreas, a vital organ involved in digestion and blood sugar regulation
- Insufficiency – indicating inadequate function or production
The term gained popularity in medical literature in the late 20th century as research into pancreatic disorders increased. Today, EPI is commonly referenced in gastroenterology, endocrinology, and dietetics.
How EPI Works: Understanding the Condition
The pancreas performs two main functions:
- Endocrine Function: Produces insulin and glucagon to regulate blood sugar.
- Exocrine Function: Produces digestive enzymes—lipase, amylase, and protease—that help digest fats, carbohydrates, and proteins.
In EPI, the exocrine function is impaired, meaning the body cannot effectively digest and absorb nutrients. This can result from several causes:
- Chronic pancreatitis
- Cystic fibrosis
- Pancreatic surgery
- Diabetes
- Aging or other chronic illnesses
Symptoms of EPI
People with EPI may experience:
- Frequent diarrhea or loose stools
- Steatorrhea (oily, foul-smelling stools)
- Unexplained weight loss
- Bloating and gas
- Fatigue due to nutrient deficiencies
Examples of EPI in Real-Life Context
| Context | Example Sentence | Tone |
|---|---|---|
| Friendly | “After talking to my doctor, I learned I have EPI, but with enzyme therapy, I’m already feeling better!” | Supportive |
| Neutral | “EPI affects the pancreas’ ability to secrete digestive enzymes, leading to malabsorption.” | Informative |
| Negative/Dismissive | “He ignored his digestive issues for years, not realizing he had EPI until it worsened.” | Cautionary |
💡 Pro Tip: Using a conversational tone helps patients relate better to medical terms. Phrases like “enzyme therapy” and “digestive support” make explanations less intimidating.
Diagnosing EPI
EPI can be diagnosed using several medical tests:
- Fecal Elastase Test: Measures pancreatic enzyme levels in stool.
- Direct Pancreatic Function Test: Measures enzyme production after hormone stimulation.
- Imaging Tests: CT scans or MRIs to detect structural pancreatic changes.
- Blood Tests: Identify vitamin deficiencies or malnutrition.
Early detection is key because untreated EPI can lead to significant nutrient deficiencies and reduced quality of life.
Comparison with Related Terms
| Term | Meaning | Key Difference from EPI |
|---|---|---|
| CF (Cystic Fibrosis) | Genetic disorder affecting lungs and pancreas | EPI can be a consequence of CF, but CF affects multiple organs |
| Pancreatitis | Inflammation of the pancreas | Pancreatitis may lead to EPI but is an acute or chronic inflammatory condition |
| Diabetes Mellitus | Disorder of blood sugar regulation | Diabetes primarily affects endocrine function; EPI affects digestive enzyme production |
| Malabsorption | Inability to absorb nutrients from food | EPI is one of several causes of malabsorption |
This table helps patients and readers differentiate EPI from related but distinct conditions, reducing confusion in medical discussions.
Treatment and Management
Managing EPI typically involves enzyme replacement therapy combined with lifestyle and dietary adjustments:
- Pancreatic Enzyme Replacement Therapy (PERT): Helps the body digest fats, carbs, and proteins
- Dietary Adjustments: Smaller, frequent meals; low-fat diets may help reduce symptoms
- Vitamin Supplementation: Fat-soluble vitamins (A, D, E, K) may be deficient in EPI patients
- Monitoring: Regular check-ups to assess nutrient levels and treatment effectiveness
Alternate Meanings of EPI
While in medicine, EPI is most commonly Exocrine Pancreatic Insufficiency, it can also stand for:
- Epinephrine (Epi): A hormone and medication used for allergic reactions or cardiac arrest
- Epidural: Refers to spinal injections used in anesthesia or pain management
💡 Tip: Context is key. In medical conversations, “EPI” usually refers to pancreatic insufficiency, but in emergencies, “Epi” might mean epinephrine.
Polite and Professional Alternatives
When discussing EPI with patients or colleagues, the following phrasing can be more approachable:
- “Your pancreas isn’t producing enough digestive enzymes.”
- “You have a condition called exocrine pancreatic insufficiency, which affects nutrient absorption.”
- “We can manage this with enzyme therapy and dietary adjustments.”
Using plain language reduces confusion and helps patients feel informed rather than intimidated.
FAQs
1. What does EPI mean in medical terms?
EPI stands for Exocrine Pancreatic Insufficiency, a condition where the pancreas does not produce enough digestive enzymes.
2. What are the main symptoms of EPI?
Common symptoms include diarrhea, fatty stools, bloating, gas, unexplained weight loss, and fatigue.
3. How is EPI diagnosed?
Doctors may use fecal elastase tests, direct pancreatic function tests, imaging scans, and blood tests to confirm EPI.
4. Can EPI be cured?
EPI is a chronic condition, but enzyme replacement therapy and dietary management can control symptoms effectively.
5. Is EPI common in children or adults?
EPI can occur at any age. Children with cystic fibrosis may develop it early, while adults often develop EPI due to chronic pancreatitis or pancreatic surgery.
6. What foods should someone with EPI avoid?
Very high-fat foods may worsen symptoms, though most patients can eat a balanced diet with enzyme support.
7. Can EPI cause vitamin deficiencies?
Yes, EPI can lead to deficiencies in fat-soluble vitamins A, D, E, and K. Supplementation is often recommended.
8. Is EPI related to diabetes?
Indirectly. Chronic pancreatic disorders can lead to both EPI and diabetes, but they affect different functions of the pancreas.
Conclusion
Understanding EPI is crucial for effective management of digestive health. With proper diagnosis, enzyme therapy, and dietary adjustments, individuals with EPI can maintain a high quality of life. Always consult healthcare professionals for personalized care, and don’t ignore chronic digestive issues—they may be an early sign of EPI.
- EPI stands for Exocrine Pancreatic Insufficiency, causing malabsorption.
- Early diagnosis through stool, blood, or imaging tests is essential.
- Treatment includes enzyme replacement, diet modification, and vitamin supplementation.
- Awareness of related conditions and alternate meanings helps reduce confusion.
Read More Related Articles:
- GMFU in Text Messages: Meaning, Mood and How to Respond (2026)
- Emphasized Mean in Text: Tone, Intent and Examples (2026)
- BFN Meaning in Texts: Is It Friendly or Rude? (2026)

Megan Foster is a thoughtful and creative content creator at Meanzy.com with a strong curiosity for language and communication. Known for her clarity and attention to detail, she simplifies confusing slang, acronyms, and modern terms into easy, relatable meanings readers can trust.